NEWS
How to Start a Food Diary
Dear Diary,
Sometimes when I eat it feels like a herd of angry buffalo have taken up residence in my gut. The rumbling, the pain, and the regret are all too familiar at this point. Maybe I just shouldn’t eat at all. Maybe that would be best. I wish it could just stop…
Okay, I might not be talking about that type of diary, but I’ve had many days in my Crohn’s journey where that could have described me. Like many people with Inflammatory Bowel Disease (IBD), I have a frustrating mix of good days and bad days. It always baffled me how I could feel good one day, but terrible the next. I wanted to know why. This started my journey of paying closer attention to what I eat, and in turn, keeping a food diary.
Why a food diary?
Our environment is everything we come in contact with on a daily basis that isn’t us. The air we breath, the things we touch, and the food we eat all make up our outside environment. If nothing in our environment impacts a disease, it should feel the same every single day. For me, and many others with IBD, this just isn’t true. In this case, we must start looking at our environment as a source of triggers for our disease.
One of the largest parts about how we interact with our outside environment is what we eat. Every day we eat a variety of different foods, from a variety of different places, that have a variety of different health effects. For me, food was an easy place to start to try to figure out some of my disease triggers. I know what I am eating every day, so why not try to see if there is any connection between what I eat, and how I feel. This led me to food journaling, and it has been an invaluable resource in helping me navigate and manage my own disease. It has given me power.
Research also backs up this idea. In one study done in 2016, one group of Crohn's patients was told to exclude either the four food types they had the highest antibodies to, while the other excluded the four food types they had the lowest antibody to. The group that excluded the foods types to which they had the highest antibodies had significantly lower disease activity and significantly higher quality of life.1 We might not have access to antibody testing, but we can certainly try to figure out what foods are worsening our disease and quality of life.
How to write a food journal
There are three main things to consider when writing a food journal: what you eat, the time you eat, and how much you eat. With these three written down, you will be able to better make connections between foods and symptoms. Let's do an example: For breakfast this morning, you ate a bowl of oatmeal with blueberries, some bacon, and a cup of coffee (I know, I know, coffee isn’t exactly known for its stellar track record in collaborating well with IBD, but it's a made up example!) How would that look?
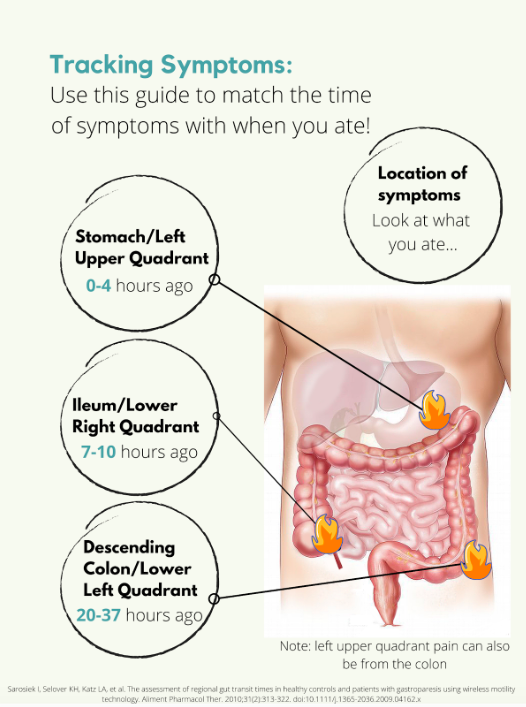
Tracking Symptoms
Symptoms are a little trickier. Say you have some pain in your lower right abdomen, how do you know what meal might have triggered you? Was it the meal you ate 5 minutes ago? 4 hours ago? The day before? For this we need to know a little bit about how long food takes to get to each different part of the intestines, also called the intestinal transit time. In a normal, healthy adult the following is accurate:
But what if you’re flaring? Diarrhea, inflammation, stricturing, and other aspects of a flare can all impact the amount of time it takes for food to get to the finish line. Some studies have been done on intestinal transit time in IBD patients, with most finding that the intestinal transit time is longer in IBD than in normal healthy subjects.2,3,4 In one patient with Crohn's disease, it took 156.2 hours for one meal to pass through. Talk about taking the scenic route! Like many other things with IBD, you are going to have to take an individual approach and problem solve to figure out how to best match symptoms and meals.
Resources
Tracking food can be done in something as simple as a spiral notebook, but there are also other options available. Here is a list of some apps you could use instead of a physical journal:
mySymptoms Food Diary & Symptom Tracker (Lite) by SkyGazer Labs LTD
Food Diary by WeCode Team
Cara Care by HiDoc Technologies
References
Gunasekeera V, Mendall MA, Chan D, Kumar D. Treatment of Crohn’s Disease with an IgG4-Guided Exclusion Diet: A Randomized Controlled Trial. Digestive Diseases and Sciences. 2016/04/01 2016;61(4):1148-1157.
Andersen K, Haase A, Agnholt J, et al. P-113 Gastrointestinal Transit Times and Abdominal Pain in Crohn's Disease. Inflammatory Bowel Diseases. 2017;23(suppl_1):S40-S41.
Fischer M, Siva S, Wo JM, Fadda HM. Assessment of Small Intestinal Transit Times in Ulcerative Colitis and Crohn's Disease Patients with Different Disease Activity Using Video Capsule Endoscopy. AAPS PharmSciTech. 2017;18(2):404-409. doi:10.1208/s12249-016-0521-3
Haase AM, Gregersen T, Christensen LA, et al. Regional gastrointestinal transit times in severe ulcerative colitis. Neurogastroenterology & Motility. 2016;28(2):217-224.
Judging Symptoms with Crohn’s
Sometimes, it feels like all gastro symptoms are inflammaotry bowel disease (IBD)-related… especially being symptomatic with IBD for so long. However, it’s not always case – which can cause a great of confusion, as well as making life just that bit more complicated!
As well as Crohn’s disease, I also have gastroesophageal reflux disease (GERD), irritable bowel syndrome with constipation (IBS-C), an internal rectal prolapse and lactose intolerance. I was diagnosed with Crohn’s disease in 2008, after several years of experience gastro-related symptoms. So, at that point, I assumed that everything I had experienced was the result of Crohn’s. What I failed to realise, and what wasn’t explained very well at the time, was that I also had GERD. I was suddenly prescribed all of this medication, without being properly informed of the purpose of each different medication.
Over time, and with the right treatment, I became more informed, and I was able to get my Crohn’s disease under control, to the point where I was deemed to be in clinical remission. This was concluded by considering blood tests for inflammation (CRP and ESR), colonoscopy and gastroscopy results, small bowel MRI scan results and faecal calprotectin results, each of them done at different frequencies over different periods of time. This happened gradually over a few years, and in the process, I learned more and more about my body. However, I began to struggle with more gastro-related symptoms, which I initially thought were a Crohn’s flare, but soon realised were not exactly the same as before my Crohn’s diagnosis. I felt bloated and constipated, I had abdominal pain, and I was passing mucus. It became clear that I most likely had IBS-C. The problem I found with IBS was that there was no quick and easy fix for it – not that there has been a quick and easy fix for Crohn’s disease, but at least I was able to take some treatment which helped control the inflammation. With IBS, I felt very much in the dark. Recommendations were an anti-spasmodic to relieve cramping, laxatives to ease constipation, and avoiding foods which seemed to make me ‘worse’. I watched what I ate very closely, and soon identified certain green vegetables as a trigger, as well as milk products, which I tried to reduce.
Little did I know, but the milk products weren’t just a trigger for worsening my IBS symptoms, but I was also lactose intolerant. I was diagnosed in 2015 – some seven years after my Crohn’s diagnosis. This only happened after one doctor felt there was something else going on and decided to test for lactose intolerance and Helicobacter Pylori infection – and thank goodness they did! I’ve managed to cut most forms of lactose completely out of my diet since, and when I can’t, I have found a lactase enzyme supplement I can take immediately before eating or drinking something containing lactose, to help me avoid those unpleasant symptoms.
I thought that was going to be it when it came to gastro problems. Then, something else came along! Originally blamed on my IBS-C, I noticed I was struggling more with constipation, despite eating a balanced and healthy diet, and doing everything else ‘right’. A couple of healthcare professionals didn’t really acknowledge my perspective, and just said I need to take laxatives permanently – something which I do take, but often feels like a ‘quick fix’ or ‘cover the wound with a plaster’, without understanding the underlying reason for these changes. Many blame IBD, plus IBS for constipation, without necessarily looking further. It sometimes feels as though assumptions are an easier option in the medical world, but not for those of us living with these symptoms. Moreover, I had observed changes beyond those I had learned to notice by living with IBD and IBS-C.
Cutting a very long story short, I ended up going for a proctogram which revealed I had an internal rectal prolapse – which is basically when your rectum folds in on itself. It wasn’t the most dignifying procedure – much like most gastro-linked investigations. Dignity often goes straight out of the window! However, this finding did explain the sharp shooting pains I had been having in my rectum, as well as the mucus I had been passing, the ‘fresh’ blood I had noticed, and why it sometimes felt as though there was a physical obstruction – because there was. The verdict was ‘there’s not much we can do’ – something I think we’re all too used to hearing. There are surgical options, but they come with risks and they more or less said they would not be considering that option for somebody of my age. So, I was sent away with pelvic floor exercises, and the notion that ‘I just have to live with it’ – which I do. At least I received an answer for the symptoms I had been experiencing, even if I don’t have an answer as to ‘why’ I have a rectal prolapse. My current hypothesis is that it is something to do with hypermobility, which has consistently been overlooked – but that’s a whole different story!
All of these different symptoms, and the conditions subsequently diagnosed, have taught me so much. I have learned to really listen to what my body is telling me – which is not easy but does improve with time. I’m not always right, but my judgement certainly seems to be stronger now, after all of these years with IBD, IBS-C, GERD, a prolapse and lactose intolerance. I am much better at distinguishing as to ‘what’ is causing ‘what’ – although it’s impossible to always be ‘right’! You just tune into what you are feeling, almost like detective work. You place pieces of the puzzle together to help you build the picture of what you think is happening. Your previous experiences and your observations guide you, alongside being proactive in terms of knowing clinical indicators, recognising new triggers, stressors or symptoms, and then being proactive in seeking the right input from the right healthcare professionals. It comes more naturally after years of having to take things into your own hands to get answers. For example, I now know that the abdominal pain and cramping that I frequently experience is when I am perhaps a little constipated as a result of IBS-C and my internal rectal prolapse; so I adjust certain parts of my diet and take additional laxatives when I begin to notice patterns changing, early on. Likewise, the ‘whale’ noises and ‘washing machine sensation’ immediately indicate that I’ve consumed something containing lactose without realising – like the time I ate a gorgeous cheesy pizza, and then realised I hadn’t taken my lactase enzyme… I suffered for the next few hours!
These conditions, in one sense, sensitise us to be more receptive to how our bodies work. I don’t think I would have been as knowledgeable or as ‘switched on’ as I am if I hadn’t been diagnosed with them – and I wish more people recognised this, particularly certain healthcare professionals. I often have grievances with professionals who rely solely on certain clinical indicators for disease remission. For example, those who just use CRP as an indicator as to whether you are in remission or not. This has happened to me in the past when I was evidently in the middle of an IBD flare, but at that point in time, I was not confident at self-managing my health. As it turned out, my faecal calprotectin was off the scale, and so some additional treatment helped me out immensely. What did I learn? Nobody knows my body better than myself. Healthcare professionals can help me the most when they listen to what I am saying, acknowledge my expertise, and then work with me to identify what is really happening, and then plan with me as to what to do to help manage symptoms so that I can get on with my life, and most importantly, have a good quality of life. So, when anybody questions what you are thinking or feeling, remind them of this point, and hopefully, they will change their approach so that it is supportive, rather than a hindrance.