NEWS
Meal Replacements and Oral Nutrition Supplements
Sometimes eating sucks. When my body hurts, I'm tired, and my gut is bloated, the last thing I usually want to do is add fuel to the fire by eating a meal. This is an unfortunate situation to be in because eating is one of those things we kind of have to do to survive. Luckily, there is a way to meet our needs without really eating. Enter the oral nutrition supplement. Calorie dense nutrition shakes designed to give you all the vitamins and minerals you need for livin’ in as little volume as possible. You can down one of these bad boys in under a minute and not have to worry about figuring out how you might fit an entire meal in your distended abdomen.
There are a lot of different nutrition supplements on the market, and it can be difficult to try to figure out which to buy. There are so many factors to consider, it can almost be overwhelming. In this article, I have tackled a few of the more common factors people consider when looking for supplements. Hopefully I have been able to provide some clarification on the differences between some of the common choices for meal replacement shakes.
Calories
The amount of calories I look for in one of these supplements depends on why I am using it in the first place. Am I trying to replace a meal? Then I would probably reach for something with a higher amount of calories. I usually try for at least 250 calories per shake, but closer to 500 calories is probably better. If I am using the shake to replace a snack, maybe 200-300 calories would be more desirable.
Some nutrition supplements come as a powder that you can mix with water or another liquid. The benefit of these supplements is that you can add as much powder as you want and customize the amount of calories to the situation. Products like Modulen IBD, Huel, Garden of Life Raw Organic Meal Shake, and Super Fuel all come as mixable powders. Garden of Life is one of the lowest calorie options I have seen, coming in at 120 calories per serving.
Most ready to drink supplements also have higher calorie options available. Ensure and Boost both make higher calorie versions of their regular nutrition shakes. You can usually tell a higher calorie shake because it will have the word “plus” in the name, i.e. Ensure Plus or Boost Plus. The big downside of these higher calorie versions is that a lot of the extra calories come in the form of sugar.
Fat
Fat is a tricky one. Often demonized, fat plays an important role as a source of energy, absorption of certain fat soluble vitamins, and managing inflammation. Certain fats are even essential, which means that we must get them from our diet. The type of fat in nutrition supplements matters. In most supplements, the fat content will be from vegetable oils. Animal fats are unusual or minimally used due to their tendency to be solid at room temperature.
Certain fats in vegetable oil, such as the Omega 6 fatty acids, are sometimes mis-labeled as pro-inflammatory. While these fats can be used by the body to create inflammatory molecules, research has shown that omega-6 fats are associated with lower or unchanged markers of inflammation. If you are somebody who is concerned about these fats, choose a supplement higher in monounsaturated fats such as Orgain or Huel. Looking for the words “high oleic” in the ingredients list is a good way to know that the oil used is high in monounsaturated fats. One supplement, Super Fuel, actually lets you add the fat to your shake yourself, so you can choose the exact type of fat you want!
Carbohydrates
There are a lot of considerations when looking at the carbohydrates in nutrition supplements. Some of the important things in my opinion are the sugar content, presence of artificial sweeteners, presence of maltodextrin, and fiber.
Sugar is an interesting one. The International Organization for the Study of Inflammatory Bowel Disease (IOIBD) says in their guidelines that there is insufficient evidence to recommend any specific change of intake of complex carbohydrates or refined carbohydrates or refined sugars and fructose. Therefore, any reason to limit sugar would have to be based on the known effects of high sugar consumption on heart health, gut health, weight gain, and other markers of health. Many of these supplements are high in added sugars, so it might be prudent to look for some of the lower sugar options such as Super Fuel, Huel, Orgain, or Garden of Life.
Some supplements contain ingredients that might be harmful in IBD patients. Specifically, maltodextrin and artificial sweeteners. Some of the low sugar supplements, such as Premier Protein, use artificial sweeteners like sucralose to replace sugar as a source of sweetness. Most supplements found in stores, including Ensure, Boost, and store brands such as Equate contain maltodextrin as a source of carbohydrates. In the IOIBD guidelines, the researchers note that it may be prudent to limit intake of both maltodextrin and artificial sweeteners. The authors also note, however, that the evidence for maltodextrin is theoretical and mostly based on animal models. Nutritional therapies that involve consuming nutrition supplements with maltodextrin have been found to be effective in IBD, so the jury is still out on maltodextrin.
Fiber is also a hot topic in IBD. Many foods considered healthy contain fiber, but many IBD patients who are flaring consider fiber to be something that aggravates their disease. Many of these supplements contain very small amounts of fiber, usually between 1-2 grams per serving. Some supplements, such as Huel, Kate Farms, and Super Fuel contain a higher amount of fiber. The general consensus from what I have researched appears to be that if you tolerate fiber, more is better. Like many other factors in IBD, fiber seems to be something to consider on an individual basis. Of note, Walmart’s brand Equate was the only supplement I looked at that had 0 grams of fiber per serving.
One thing to note is that some supplements include blends of fruits, vegetables, and other plant compounds. Orgain, Garden of Life, and Kate Farms all include these special blends, likely to try to mimic the benefits of eating whole foods. Other supplements, such as Huel and Super Fuel are made primarily from whole foods.
Protein
The protein needs of an IBD patient are increased during a flare. Protein is needed to help repair damaged tissue and maintain muscle mass, among many other functions. I think it is important to make sure that the nutrition supplement you choose has the protein your body needs to function optimally.
Most supplements have enough protein to meet your body's needs. A little trick I use is to try to shoot for 20% of calories from protein. You might need to whip up your phone calculator in the store, but the math isn’t too hard. First you would take the grams of protein and multiply it by 4, because there are 4 calories in every gram of protein. Then, all you need to do is divide the number of calories of protein by the total calories and multiply by 100 to get the percent!
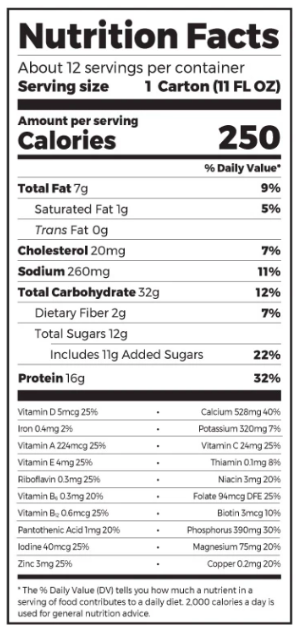
Let's do an example with Orgain’s Nutritional Shake:
Looking at the bottom, we see Orgain has 16 grams of protein per serving.
Step one would be to multiply 16g by 4 to get the number of calories, which would be 64 calories of protein.
Step two, would be to divide the number of protein calories by the number of calories in a serving, which can be seen at the top of the nutrition facts label.
We would do 64 calories divided by 250 calories and get 0.256.
The final step, to get a percentage, would be to multiply by 100 to make that number a percentage. So, .256 multiplied by 100 is 25.6%.
25.6% is more than 20%, so Orgain would pass my little test!
Some of the higher protein supplements out there are Huel, Ensure Enlive, and Premier Protein, and Garden of Life. It is important to note that if you aren’t in a flare, your protein needs are likely no higher than the rest of the population.
Carrageenan
Carrageenan is an emulsifier used to help the ingredients in shakes mix smoothly. It has also been shown to cause a variety of negative effects in animal models, such as increased blood in stool, increased inflammatory markers, and lesions in the bowel. For these reasons, and some small scale human research, IOIBD also states that it may be prudent to reduce intake of processed foods that contain carrageenan in both UC and Crohn’s Disease. Most of the supplements found in stores, such as Ensure, Boost, and store brands such as Equate use carrageenan in their nutrition supplements. If carrageenan is something you wish to avoid, you can usually locate it at the bottom of the ingredients list. You can see it is the last ingredient in Ensure Plus.
To Conclude
I wish I could add more detail, but I don’t want to break your scroll wheel. The most important thing to do when looking for an oral nutrition supplement is to take a look at the nutrition facts label and make sure you are comfortable with the nutrition content and ingredients in your shake. I usually try to look for higher protein and fiber, and lower added sugars while avoiding sucralose, maltodextrin, and carrageenan. Oh and the shake has to taste good too. Could you imagine not wanting to eat anything and reaching for a shake that didn’t even taste good? Neither could I. Considering all that, I usually go for Orgain nutritional shakes. They fit my goals as far as cost, taste, and nutritional content are concerned.
Another option is to try to make your own shake in a blender. It can be pretty easy to toss some oats, a banana, and a few scoops of peanut butter together and have a tasty, nutritionally dense smoothie to sip on. You even save some money that way too! At the end of the day, store bought shakes or homemade, oral nutrition supplements can be a great way to give your body the fuel it needs to function when you don’t feel like making or eating a meal.
Digestive Disease Week: Role of Diet, Lifestyle, and Environment in IBD
I thoroughly enjoyed attending Digestive Disease Week’s session on Role of Diet, Lifestyle, and Environment in Inflammatory Bowel Disease. Let's start from the beginning and understand why studies surrounding diet, lifestyle, and environment are so important in understanding IBD.
IBD affects nearly 3 million Americans and over 200,000 Canadians. IBD is an immune-mediated disease that occurs due to certain, unknown environmental exposures in those with underlying genetic predispositions. Research on environmental exposures is needed to discover what environmental factors may contribute to an individual receiving an IBD diagnosis. This research will not only create an overall improved understanding of IBD, but also contribute to reducing the onset of IBD as well as cures for IBD.
Ultra-Processed Foods and Risk of Crohn’s Disease and Ulcerative Colitis
Two speakers in this session I found extremely interesting, the first being Dr. Chun-Han Lo. Dr. Lo reviewed his study on ultra-processed foods and risk of Crohn’s Disease and ulcerative colitis. The Western diet is thought to increase the risk of IBD through changes in the gut microbiome which can trigger immune function when compared to the Mediterranean diet.
Foods were separated into four categories from least to most processed:
Unprocessed
Processed culinary ingredients
Processed foods
Ultra-processed food products
Dr Lo explains that right now, it is widely known that higher consumption of ultra processed food products is associated with all-cause mortality, cardiovascular disease, metabolic syndrome, obesity, and cancer. Agents and thickeners, that are often added to ultra-processed food products, were also examined. The study aimed to examine the associations between ultra-processed food products and the risk of incident of Crohn’s Disease and ulcerative colitis.
The results indicated that higher consumption of ultra processed food products, specifically ultra processed grain foods and fat and sauces, was associated with an increased risk of Crohn’s Disease. Additionally, emulsifiers and thickener containing foods increased the risk of Crohn’s Disease. No subgroups had an association with risk of ulcerative colitis. This differentiates the impact food may have on Crohn’s Disease versus ulcerative colitis, furthering complexifying IBD. Further studies are needed on the effect of ultra processed food products in patients with established IBD may be warranted.
Although you may not be surprised by the results, studies like these are so important to allow room for more niche research and continue to allow researchers and doctors to understand the WHY behind IBD. As a Crohn’s Disease patient with many food intolerances, I am excited to see research surrounding diet and quality of food. There is little research backing the quality of food, and many suggest following a specific diet such as low FOD-map, gluten free, dairy free, among many others. It’s extremely exciting to see additional research surrounding foods, specifically processed versus unprocessed foods. My hopes are that this study can contribute to encouraging people to eat better quality foods and, in turn, reduce Crohn’s Disease diagnoses. Further, my mind jumps to future research covering whether reducing ultra processed food products after an IBD diagnosis could help treatment and management of disease.
Development of a Composite Environmental Score to Predict Age of Onset and Outcomes in IBD
Dr. Nidah Shabbir Khakoo spoke on the development of a composite environmental score to predict age of onset and outcomes in IBD. Specifically, Dr. Khakoo focuses on the fact that many environmental exposures associated with IBD are increasingly seen with Westernization. The study aimed to explore the relationship between individual environmental exposures and the age of onset of IBD. This study is extremely important in order to come to the understanding of what can cause a person to be diagnosed with IBD earlier in life, rather than later.
As someone with IBD, I have frequently wondered what environmental exposures in my life have caused my IBD to have an earlier onset? Why did I receive my IBD diagnosis in my early twenties compared to others that are diagnosed in their fifties? These studies are crucial to understand potential causes for earlier disease onset and overall understanding of IBD.
This study was administered on adult patients previously diagnosed with IBD. An environmental survey that queried age-dependent and lifetime exposures to various environmental factors were given among the participants to identify the environmental exposures each subject has had throughout their lifetime while looking at the age of their diagnosis. It is important to note that this study had a large number of hispanics, an underrepresented group in IBD research. The study looked at the age of disease onset, specifically comparing hispanics vs non-hispanics and Crohn’s disease vs ulcerative colitis patients.
Earlier Ulcerative Colitis Onset:
US Born
C-section Delivery
Fewer bathrooms
Decreased housing density
Ex-smokers
No farm contact
Earlier Crohn’s Disease Onset:
US Born
Water source - plastics
Fewer bathrooms
Decreased housing density
Smokers
Dr. Khakoo shares that the environmental score presented explains a greater amount of the variation in the age of UC onset than Crohn’s Disease onset. Additionally, weighted and not-weighted scores did not predict disease location, presence of extraintestinal manifestations, likelihood of surgery or hospitalization, or number of biologics needed. Certain environmental exposures, such as bottle feeding, showed opposing effects in ethnic groups with IBD, leading to assume that cultural and socioeconomic factors may influence disease onset.
These results give a baseline that other research needs to build off of. It is becoming increasingly evident that ethnicity differentiates environmental factors contributing to IBD and more research is needed to understand these differences. I’m looking forward to hearing of future studies regarding this subject and am hopeful more nuances regarding environmental exposures and the timing of IBD onset will be discovered.
It was great to hear from multiple experts about diet and environmental factors relating to IBD. I think that the data so far shows that there is a lot of work to do to understand what environmental factors contribute to IBD. I am looking forward to seeing future studies dive more in-depth to discover the causes of IBD. I am incredibly grateful to have heard from Dr. Chun-Han Lo and Dr. Nidah Shabbir Khakoo, and am confident these studies will have a large influence on future research on Inflammatory Bowel Disease.
IBD, Mental Health, and Diet
Have you ever had a gut feeling before? Maybe you’ve had butterflies in your stomach when taking a risk, or felt something in the pit of your stomach when receiving bad news. Are these just idioms, or is there something else there? On my journey to become a registered dietitian, the connection between food and physical health is a common theme. Something we talk about much less is the connection between food and mental health. While Inflammatory Bowel Disease (IBD) is often thought of as a physical disease, the mental impact cannot be ignored. In my opinion, we don’t talk enough about the IBD and mental health connection, and we certainly don’t talk enough about how food can play a role in this aspect of our disease.
Mental Health and Gut Health
What does gut health have to do with mental health? Strap on your helmet, it's time for a crash course in the connection between gut health and the brain. The gut has over 500 million nerves, which serve as a two way communication system with the brain. If your gut isn’t happy, you better believe it is going to let its good friend the brain know about it. Our guts are also responsible for producing neurotransmitters, which help to regulate physical and mental functions of the body. One important neurotransmitter that regulates mood, serotonin, is produced 95% in the intestines! Another one, GABA, can be produced by the friendly bacteria in the gut, and can help reduce feelings of anxiety, depression, and fear.
Mental Health and IBD
As you can see, the gut and the brain are basically best buds. But what does that mean for people whose guts are broken more frequently than the McDonalds ice cream machine? Unfortunately, IBD patients are at an increased risk for developing anxiety and depression, and frankly, can you blame us? We are forced to bear the burden of a lifelong chronic disease, often being diagnosed during some of the most mentally vulnerable stages of our lives. High school is hard enough without explaining why you spend half of every class in the bathroom. It might seem like the connection between intestinal health and brain health is bad news, but there is a silver lining. If we can change the health of our gut, we can change the health of our brain.
Diet and Mental Health in Healthy Individuals
In healthy individuals, certain diets have been shown to increase feelings of wellbeing, reduce feelings of depression, and improve psychological health. Both individual foods such as fruits and vegetables, as well as dietary patterns such as the mediterranean diet, have been linked to these benefits. Some foods are also associated with worse mental health. Sugar has been linked with mood disorders and depression. Excess sugar consumption is also associated with dysbiosis, a shift in the composition of the gut bacteria from helpful to harmful species.
Diet and Mental Health in IBD
In a study presented at Digestive Disease Week 2020, researchers categorized IBD patients into two groups, a high sugar group (>100 grams per day) and a low sugar group (<100 grams per day). They found that those in the high sugar group had increased feelings of fatigue, trouble with social engagement, feelings of depression, and trouble relaxing compared to IBD patients in the low sugar group.
It is important to note that sugar containing whole foods such as fruit have been strongly linked to positive health outcomes, and should be considered differently than sugars from processed foods. Added sugars from processed foods such as soda or candy are associated with an unhealthy gut, and worse overall health.
I think this is such an important study, not only because it has practical implications for IBD patients, but also because it opens doors for patients to take control of their own mental health. I don’t think I've ever had a conversation with any GI doctor about mental health, despite the increased risk we carry with IBD. Until that changes, it is reassuring to know that we have the option to eat in a way that is associated with good gut health, and therefore good mental health.
References
Choi K, Chun J, Han K, et al. Risk of Anxiety and Depression in Patients with Inflammatory Bowel Disease: A Nationwide, Population-Based Study. J Clin Med. 2019;8(5):654. Published 2019 May 10. doi:10.3390/jcm8050654
Knüppel, A., Shipley, M.J., Llewellyn, C.H. et al. Sugar intake from sweet food and beverages, common mental disorder and depression: prospective findings from the Whitehall II study. Sci Rep 7, 6287 (2017). https://doi.org/10.1038/s41598-017-05649-7
Stranges S, Samaraweera PC, Taggart F, Kandala NB, Stewart-Brown S. Major health-related behaviours and mental well-being in the general population: the Health Survey for England. BMJ Open. 2014;4(9):e005878. Published 2014 Sep 19. doi:10.1136/bmjopen-2014-005878
Parletta N, Zarnowiecki D, Cho J, et al. A Mediterranean-style dietary intervention supplemented with fish oil improves diet quality and mental health in people with depression: A randomized controlled trial (HELFIMED). Nutr Neurosci. 2019;22(7):474-487. doi:10.1080/1028415X.2017.1411320
Brown K, DeCoffe D, Molcan E, Gibson DL. Diet-induced dysbiosis of the intestinal microbiota and the effects on immunity and disease [published correction appears in Nutrients. 2012 Oct;4(11)1552-3]. Nutrients. 2012;4(8):1095-1119. doi:10.3390/nu4081095
Bone Broth: Nature's Multivitamin
It seems that #guthealth has become popular in the wellness space over the past year or so. With more awareness of IBS, Leaky Gut, SIBO, and many other bacteria imbalances in the gut being displayed through the media, there has been an increase in remedies that are bound to “fix” all gut issues. I am an advocate for taking preventive, healing measures to get to the root cause and work towards better overall health - not necessarily relying only on medication. However, these so-called remedies are not a “cure-all.” While diet plays SUCH a significant role in gut health, but there are far too many factors that contribute to overall gut health that are often overlooked. In terms of IBD, chronic inflammation is exactly what it sounds like – chronic. Those who are facing this issue often try several things to help tame inflammation and improve their health, but there is not one “cure” that will work for everyone. Many things can trigger inflammation, and those are different for each person. Common examples include: food sensitivities / intolerance, stress, hormone imbalances, and mental strain. All of which can cause added irritation and stress to our system which results in inflammation and often the inability to turn off our “fight” mode.
While stress is a main component of a suppressed immune system there are plenty of other factors that influence the lining of the gut itself - factors such as prolonged exposure to antibiotics, inflammatory foods, toxins, etc. Eventually, if the impact of these factors pile up, the lining of the gut can suffer and result in permeability issues that may cause excessive inflammation due to malabsorption of food and minerals.
One thing I am currently working on in terms of my Crohn’s Disease is repairing the lining of the gut. Due to years of antibiotic treatment, inflammatory foods, and chronic stress, the lining of my gut has taken a toll and is not as impermeable as it should be. I am planning on writing a separate post about my current protocol, as well as the lifestyle changes I am implementing, but for now, I would like to talk about two things I have added into my routine and their role in digestive healing.
There is a chance that either in your research, scrolling through social media wellness accounts, or talking with your doctors, you have heard about bone broth. Many healing diets such as GAPS and the Specific Carbohydrate include this as part of the beginning protocol, and for a great reason! Nutrients and minerals in bone broth are essential to improve and heal the lining of the gut. These nutrients help decrease inflammation, balance good / bad bacteria ratios, and increase the immune response. Bone broth is nutrient-dense, easy to digest, rich in flavor and boosts healing within the entire body – what’s not to love!
What exactly is Bone broth?
You may think of broth that your mom used to have you sip when you were sick as a kid, typically what is used in homemade soups. However, bone broth is much different – it is nutrient-dense, thicker, and in my opinion, SO much better. Bone broth is the result of steeping the entire bone remains of the animal (beef, lamb, pork, chicken, etc.); including the bone, marrow, tendons, ligaments, etc. By including all of these components, the amount of nutrients found in this broth is significantly high compared to regular broths. Simmering using the “nose to tail” method of the animal protein source enables the bones and ligaments to release healing compounds like collagen, proline, glycine, and glutamine that are transformative for your health (1). Bone broths contain minerals and essential amino acids in forms that are easy for our body to absorb. Some of the minerals included are; calcium, magnesium, phosphorus, sulfate – all of which are often sold as pricey supplements and used to reduce inflammation, joint pain, and arthritis.
It is important to be mindful of the kind of bone broth you are consuming. Meaning, not all store-bought broth is created equal. If you’re not going to make your bone broth at home (from scratch), it is crucial to check the ingredients of what you are purchasing in the store! Like many other products, manufacturers like to sneak in monosodium glutamate (MSG), which is recognized as a meat flavor but is actually a neurotoxin – and as mentioned earlier, toxins affect the gut! When looking at the ingredients list, you should seek out whole, organic ingredients such as the bone broth (filtered water and animal bones), organic vegetables, and minimal spices. Try to stay away from added preservatives because to reap the full benefits of bone broth it is best to consume it in its most natural form – as our ancestors would have prepared it!
Overall, bone broth is a great place to find all of the valuable amino acids, collagen, gelatin, and trace minerals. There are dozens of different nutrients found within bone broth, many of which can’t be obtained easily from other commonly eaten foods! I am a firm believer in using food as medicine and consuming as much nutrient-dense food as possible. Broth is one of the easiest ways to check those nutrient boxes off without having to consume a massive pile of veggies in one sitting! By regularly drinking bone broth, or using it in recipes, you can promote healthy gut integrity while reducing inflammation and permeability. Now let’s dive into some other benefits from regularly consuming bone broth, shall we?
1. Protects Joints
I’ve already mentioned the anti-inflammatory properties that broth has due to the nutrients. But one of the BEST components found in this broth? Collagen. Bone broth is one of the world’s best sources of natural collagen – a protein found in vertebrae animals; in their bones, skin, cartilage, ligaments, tendons, and bone marrow. Collagen is very beneficial for the growth of hair, skin, nails, and bone health (2).
As we get older, our joints naturally experience depletion resulting in loss of flexibility. Supplementing with collagen matters because as we age, cartilage diminishes. As the broth simmers, animal parts release collagen and it becomes readily absorbable to help restore cartilage.
Another valuable component in the stock is gelatin. Gelatin acts like a soft cushion between bones that helps them move smoothly without friction. It provides the building blocks that are necessary to form and maintain strong bones. Significant amounts of both collagen and gelatin form and reform connective tissue to help take the pressure off of aging joints and supports healthy bone mineral density. It’s never too early to start taking preventive measures to make joint pain less problematic as you get older!
2. Boosts Detoxification
As I have previously mentioned, in our Western World, the average person is exposed to a variety of environmental toxins, pesticides, artificial ingredients and chemicals. The human body is amazing in terms of having its own means of detoxification from heaving metals and other toxins. However, it has a hard time keeping up when it is flooded with large amounts of chemicals. Much like if you were to procrastinate and become swamped with homework, you’re suddenly overwhelmed and may not perform your best on the task at hand. Bone broth is considered a powerful agent in detoxification because it helps the digestive system expel waste and promotes the liver’s ability to remove toxins. It also helps to maintain tissue integrity and improves the body’s use of antioxidants.
Stock contains potassium and glycine – both of which support cellular and liver detoxification. By supplying sulfur (especially with added vegetables, garlic, and herbs) and glutathione, an agent that lowers oxidative stress, detoxification is boosted. Glutathione helps with the elimination of fat-soluble compounds, especially heavy metals such as mercury and lead. It also aids in the use of antioxidants, the absorption of various nutrients, and with liver-cleansing functions! With the increased intake of essential minerals that bone broth stimulates, the minerals act to remove toxins by stopping heavy metals from attaching to mineral receptor sites. If they can’t bind, they can’t mess with our systems!
3. Supports Immune System Function
I have briefly mentioned at various times the permeability of the gut lining, inflammation, and a suppressed immune system. All of which contribute to multiple issues with what would generally be a healthy inflammation response.
Leaky gut syndrome occurs when undigested particles from foods seep through tiny openings in the weakened intestinal lining and enter the bloodstream. The immune system detects these invaders and becomes hyperactive to regulate the body. The hyperactivity increases inflammation and leads to dysfunctions all over, not just in the gut where the primary issue lies. The immune system releases high levels of antibodies that cause an autoimmune–like response and begins to attack healthy tissue. Individuals that already have a compromised autoimmune system, such as IBD patients, may suffer considerably more damage from a response because the system believes the particles in the bloodstream to be much more of an invader than a conventional system may.
Bone broth is observed to be one of the most beneficial foods to consume to restore gut health and therefore support immune system function and healthy inflammatory response. Collagen, gelatin, and the amino acids proline, glutamine, and arginine help seal the openings in the lining and support what is known as “gut integrity” – the intactness of the lining of the intestine to maintain its structure and function.
The amino acids and anti-inflammatory benefits create a perfect atmosphere for powerful immune-boosting to occur!
4. Good for the Gut
Bone broth stock is easily digested and soothing to the digestive system, unlike many other foods, which can be challenging to break down. Those with food sensitivities and intolerance (such as wheat or dairy) already have a hard time consuming many foods that may be considered “inflammatory.” Therefore, it is essential to look after the integrity of the gut, so vital nutrients are absorbed to support other bodily functions and overall health. After all, food is only useful if we have the means of absorbing its nutrients.
Bone broth has also been found to help heal the lining of the gastrointestinal tract. Critical components for digestion support that are found in bone broth include - collagen (proline / glycine), gelatin, and glutamine. Although there are many other beneficial minerals contained, these are most helpful to many IBD patients that have difficulty successfully digesting and passing bowel movements.
A healthy digestive tract consists of a single, tight layer of epithelial cells, a thick mucus layer, and a diverse group of microbes (bacteria in the gut). Gelatin is a significant component when it comes to the lining of the digestive tract because it supports a healthy lining of mucus within the system. The water is absorbed within to help maintain the layer of mucus that blocks gut microbes from the intestinal barriers. By drawing fluid into the intestine, the motility of the gut is improved, and healthy bowel movements are supported.
Collagen is another important component because it contains two essential amino acids: proline and glycine. Proline is necessary for the formation of collagen, and glycine works to improve digestion by increasing gastric acid secretion. Studies are currently being conducted and have shown that individuals with IBD, mainly Crohn's, are more likely to suffer from low stomach acid (3). Because the proper pH of the stomach signals the continuum of the digestive cascade, many people with low stomach acid face difficulty processing meals efficiently.
Summary
I know that was a lot of information, some of which may not have processed the first time reading it through - but that’s perfectly okay! Luckily you don’t need to know the names of all the essential amino acids found in bone broth to reap the benefits. I included this information because I know when I am learning about a new “supplement” that can improve my health, I’d like to know exactly how it works and why it is good. Many others like me enjoy doing their research to learn more, but others enjoy knowing the benefits, plain and simple!
So, another run down. When taken consistently, bone broth is exceptionally nutritious and works diligently to repair multiple components of your digestive tract. In addition to this, benefits are often seen through support in joint and bone health, hair / skin / nails, and detoxification processes of other organs within the body. It truly is impressive how functional this food is - hence, the nickname “nature’s multivitamin!”
I highly recommend giving this a try, whether you buy it from the store or experiment with making your own. I believe it’s wonderful! I drink mine first thing every morning, and it’s become something I look forward to - some people drink coffee, I drink bone broth (with an added scoop of collagen)! I hope you found this article informative and it piqued your interest to try something new, or reintroduce something back into your routine!
Stay Lovely,
Erin
IBD Diets: Gluten Free for Crohn's and Colitis
By Leah Clark
Because of the popularity of Hollywood fad diets, the term 'gluten-free' has become more and more popular over the past decade. While not necessarily intending to do so, this trend actually brought great change to individuals suffering from celiac disease, non-celiac gluten sensitivity, and inflammatory bowel diseases. With new food products coming to market and more menu items coming to restaurants, it has provided a new way for people that cannot eat gluten to experience food. As someone that was diagnosed with both celiac disease and #Crohn's disease ten years ago, I can confidently say I know my way around a nutrition label. That being said, not everyone that is on a gluten free diet, or that is planning on starting one, knows what to do. When discussing your treatment plans for your IBD with your doctor, discussing diet changes should not be forgotten. So, is going gluten free right for you?
Bacon, eggs, potatoes...who says living a gluten free lifestyle means giving up your favorite breakfast foods!
What is gluten?
With all these terms of gluten free, gluten sensitive, wheat-free, gluten-friendly, and more, it can be confusing to know what it all means! Isn't flour gluten, or is it any grain? To start with the basics of a gluten free diet, one has to know what to look for. Gluten is the proteins found in wheat, rye, and barley. So when on a gluten free diet, wheat, rye, and barely are the foods to avoid.
How to read labels
Okay, so know that I know what to avoid, what are the necessary steps to ensure that I don't eat the wrong foods? Check labels on everything. Even if you think something may be gluten free, it never hurts to read the nutrition labels. Certain foods don't have labels, such as fruits and vegetables; however, these foods do not consist of any other ingredients other than what they are called-apples, carrots, oranges, etc. Foods that are made with other ingredients, such as cereal, pasta, and crackers, are foods that need to be checked. Luckily, most companies are good about food labeling, so boxes will often say "Gluten Free" or "Contains: milk, soy, and wheat."
However, sometimes there are tricky labels that you need to look out for. For example, the cereal Rice Krispies is not #glutenfree. The ingredients include rice, sugar, salt, malt flavor, and vitamins and minerals. The key word here is malt. Although the other ingredients are okay, the malt flavor is not. Malt is a tricky word because it is not wheat, rye, or barely; however, malt is a derivative from barley. Therefore, Rice Krispies are not gluten free. Words like malt extract, malt flavoring, barley malt, wheat-germ, and non-gluten free oats, are words to look out for.
What foods can I eat?
A good rule of thumb is to stick to foods that are labeled gluten free, or are"natural" foods. By natural, I mean foods that are not made with large amounts of ingredients. A good starting gluten free grocery
list could include:
Fruit-apples, bananas, kiwi, oranges, grapes, strawberries, raspberries, blueberries, plums
Vegetables-carrots, corn, green beans, lettuce, spinach, broccoli, radishes, celery, zucchini
Milk-can be almond, dairy, soy, cashew
Protein-lean meats, chicken, eggs
Dairy products-cheese, gluten free yogurt, butter, cottage cheese
Grains-white or brown rice, gluten free oatmeal, gluten free breads and pastas
Gluten free pizza? Yes please! Restaurants have gotten better at properly preparing gluten free dishes, including delicious pizza, to make it easier for people to enjoying going out to eat.
Gluten free diet can not only be good for your gut, but also for other parts of your body because of how healthy a gluten free diet can be. Many of the foods listed are healthy in their nature, like lean meats, fruits, and vegetables. However, just because something says "gluten free," does not mean it is part of a healthy diet. Sure, chocolate is gluten free, but if all you ate was chocolate, would that be the best way to go on a gluten free diet? Probably not.
But I thought gluten free foods always tasted bad?
A common misconception about gluten free food is that it tastes gross. While yes, there are some bad gluten free food products out there, this is no different than there being bad gluten food. It all depends on your preferences and experimenting with different brands. Making home-made gluten free brownies is not as simple as using a Pillsbury box recipe of 'normal' brownies (although, there are some Pillsbury gluten free baking products that taste great). The point is to try new brands and baking techniques that work for you. I've spent the last ten years of my life finding my favorite brands of pastas, crackers, and bread, and I can honestly tell you, it wasn't I traveled to an entirely different country and tried their gluten free bread that I found my favorite. Gluten free food can taste just as good, if not better, than the food you're used to! It just takes some time and preparation.
How do I know if gluten free is right for me?
Honestly, it all depends on what you and your doctor think is best for you. I had to go gluten free because I was diagnosed with a disease that literally required me to. Yet, I know several people with Crohn's or colitis that have gluten free diets that do not also have celiac disease. In short, if eating certain foods make you feel bad, do not eat those foods! There are other foods I avoid even though they are gluten free, such as popcorn and caffeinated sodas, because I know they upset me. It truly depends on each person and if it is going to help with your treatment for IBD.