NEWS
The Patient-Doctor Relationship
Why is a good relationship with the doctor important for patients?
Have you ever considered how your relationship with you doctor affects your health?
“There is no cure. Only control of the disease symptoms”. How many times have you heard this? How harsh does it sound, especially the first time?
Are you ready to build a new relationship, a completely different relationship with your doctor? This relationship will be unlike any other relationship and certainly no one has experienced it again until the time of diagnosis.
This is a long-term relationship that will evolve over time. Your doctor will know many things about your personal life, your job, your family, etc. Above all, however, over time, he or she will learn YOU, and your personality.
And why this is important?
As a patient you have to break down the wall around you and allow the doctor to enter your world, the world of your disease and how you experience it, even for a while. Of course, the doctor must have the empathy required for that.
This will not happen overnight. It may take years to build this relationship. As this relationship begins to build, you will feel the doctor as a member of your family, you will share with him or her important moments.
Is always the relationship between patient and doctor like that?
Unfortunately, no - however, I deeply appreciate those doctors who patiently and carefully support patients with chronic diseases. It’s nice to see a person being 100% present.
Journaling with IBD: A Focus on Mental Health
During 2020’s intermittent quarantine, what has brought me more solace than anything is the act of journaling. As someone who was diagnosed with Crohn’s disease during the pandemic, much of my hospital experience was drastically different than others. Increasingly isolated from my loved ones, I could feel the weight of my diagnosis crushing me, the four walls of my hospital single closing in.
For IBD patients specifically, mental health is tied so closely to our physical health. I’ve had days where my physical flare-ups make me double over; it’s no coincidence that those same days, my mood swings and sensitivity levels are out of control. In fact, this phenomenon is so common that there’s an actual term for it: the gut-brain connection.
The gut-brain connection refers to how changes in our gut can have drastic impacts on how we feel and behave. Many tend to dichotomize our bodily systems, finding it hard to believe that our behaviors and moods can be swayed by what we eat and how our gut reacts. This is explained by what’s called ‘bi-directional’ communication, in which our gut and brain talk to each other using different pathways.
Re-focusing energy is powerful. With enough time, journaling can become a way to channel your energies into finding peace and introspection. What’s best about all this is that journaling can take any form you want it to. It’s simply a way to get your thoughts out on the page. Humans absorb so much information and stimuli during their waking hours; life, as it turns out, can be overwhelming at any point in time, regardless of an IBD diagnosis or not.
Journaling should be a way to relieve stress, a way to declutter your mind. I’ve found it especially helpful to process my physical and mental pain; even doodling can help distract your mind for a few minutes. Especially for patients with IBD, a journal can be a place to record symptoms, reflect on treatments, or even track what foods you’re eating (Check out this article on how to start a food diary by David, a 2021 CCYAN Fellow!)
All you need is a notebook, even just a piece of paper, and a pen or pencil. Some people find it helpful to pair a journaling session with a few minutes of meditation: this is your choice! Whatever makes you feel the most grounded and relaxed.
Here are a few journaling prompts to get you started:
How are you feeling right now?
What does your body need?
What is giving you energy? What is taking your energy?
What are you grateful for, at this moment?
What are some themes in your life right now? (rest, peace, healing, etc.)
Things that feel heavy today; things you can try and release today.
What do you need to let go of in order to move forward and grow?
What beliefs and assumptions are holding you back?
What do you have to be proud of?
Where are you feeling stuck? Where are you feeling growth?
How to Start a Food Diary
Dear Diary,
Sometimes when I eat it feels like a herd of angry buffalo have taken up residence in my gut. The rumbling, the pain, and the regret are all too familiar at this point. Maybe I just shouldn’t eat at all. Maybe that would be best. I wish it could just stop…
Okay, I might not be talking about that type of diary, but I’ve had many days in my Crohn’s journey where that could have described me. Like many people with Inflammatory Bowel Disease (IBD), I have a frustrating mix of good days and bad days. It always baffled me how I could feel good one day, but terrible the next. I wanted to know why. This started my journey of paying closer attention to what I eat, and in turn, keeping a food diary.
Why a food diary?
Our environment is everything we come in contact with on a daily basis that isn’t us. The air we breath, the things we touch, and the food we eat all make up our outside environment. If nothing in our environment impacts a disease, it should feel the same every single day. For me, and many others with IBD, this just isn’t true. In this case, we must start looking at our environment as a source of triggers for our disease.
One of the largest parts about how we interact with our outside environment is what we eat. Every day we eat a variety of different foods, from a variety of different places, that have a variety of different health effects. For me, food was an easy place to start to try to figure out some of my disease triggers. I know what I am eating every day, so why not try to see if there is any connection between what I eat, and how I feel. This led me to food journaling, and it has been an invaluable resource in helping me navigate and manage my own disease. It has given me power.
Research also backs up this idea. In one study done in 2016, one group of Crohn's patients was told to exclude either the four food types they had the highest antibodies to, while the other excluded the four food types they had the lowest antibody to. The group that excluded the foods types to which they had the highest antibodies had significantly lower disease activity and significantly higher quality of life.1 We might not have access to antibody testing, but we can certainly try to figure out what foods are worsening our disease and quality of life.
How to write a food journal
There are three main things to consider when writing a food journal: what you eat, the time you eat, and how much you eat. With these three written down, you will be able to better make connections between foods and symptoms. Let's do an example: For breakfast this morning, you ate a bowl of oatmeal with blueberries, some bacon, and a cup of coffee (I know, I know, coffee isn’t exactly known for its stellar track record in collaborating well with IBD, but it's a made up example!) How would that look?
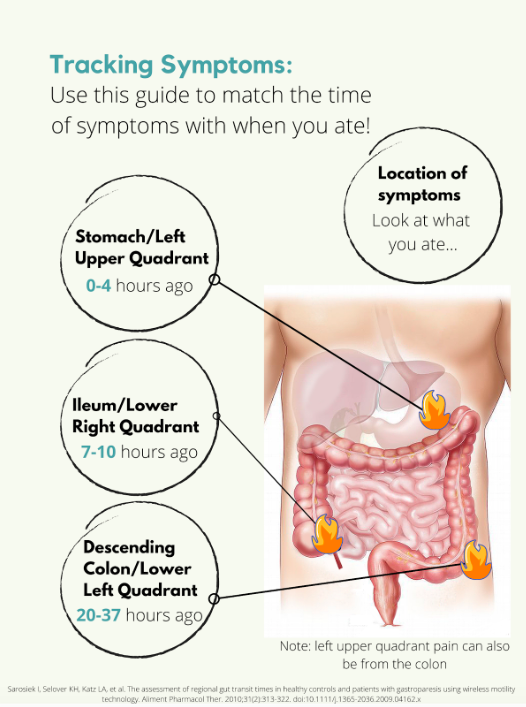
Tracking Symptoms
Symptoms are a little trickier. Say you have some pain in your lower right abdomen, how do you know what meal might have triggered you? Was it the meal you ate 5 minutes ago? 4 hours ago? The day before? For this we need to know a little bit about how long food takes to get to each different part of the intestines, also called the intestinal transit time. In a normal, healthy adult the following is accurate:
But what if you’re flaring? Diarrhea, inflammation, stricturing, and other aspects of a flare can all impact the amount of time it takes for food to get to the finish line. Some studies have been done on intestinal transit time in IBD patients, with most finding that the intestinal transit time is longer in IBD than in normal healthy subjects.2,3,4 In one patient with Crohn's disease, it took 156.2 hours for one meal to pass through. Talk about taking the scenic route! Like many other things with IBD, you are going to have to take an individual approach and problem solve to figure out how to best match symptoms and meals.
Resources
Tracking food can be done in something as simple as a spiral notebook, but there are also other options available. Here is a list of some apps you could use instead of a physical journal:
mySymptoms Food Diary & Symptom Tracker (Lite) by SkyGazer Labs LTD
Food Diary by WeCode Team
Cara Care by HiDoc Technologies
References
Gunasekeera V, Mendall MA, Chan D, Kumar D. Treatment of Crohn’s Disease with an IgG4-Guided Exclusion Diet: A Randomized Controlled Trial. Digestive Diseases and Sciences. 2016/04/01 2016;61(4):1148-1157.
Andersen K, Haase A, Agnholt J, et al. P-113 Gastrointestinal Transit Times and Abdominal Pain in Crohn's Disease. Inflammatory Bowel Diseases. 2017;23(suppl_1):S40-S41.
Fischer M, Siva S, Wo JM, Fadda HM. Assessment of Small Intestinal Transit Times in Ulcerative Colitis and Crohn's Disease Patients with Different Disease Activity Using Video Capsule Endoscopy. AAPS PharmSciTech. 2017;18(2):404-409. doi:10.1208/s12249-016-0521-3
Haase AM, Gregersen T, Christensen LA, et al. Regional gastrointestinal transit times in severe ulcerative colitis. Neurogastroenterology & Motility. 2016;28(2):217-224.
How Toxic Productivity Can Affect Chronic Illness
“The grind never stops” is a quote I’m sure all older gen-z and younger millennials have heard. Hustle culture is like the monster hiding under our beds just waiting to attack us the moment we dangle our foot off the bed. It’s the scary email we try to avoid, but eventually have to acknowledge is there. Our society places a great amount of pressure, on our generation specifically, to work hard and constantly strive for a lifestyle in which we are operating at an “optimal level”. This is deemed as success and this version of success should always be at the forefront of our minds and influence all decision making. Participating in this hyper productive hustle culture is difficult enough for the average person to achieve, but what does it look like for people that live with chronic illness?
To put it simply, living with chronic illness(es) is hard. Personally, it is the most difficult thing I have ever experienced. With symptoms like chronic fatigue, anemia, and anxiety etc., paired with frequent doctor's appointments and stigma, one could imagine that it is virtually impossible for chronically ill people to participate in hustle culture. Unfortunately, being in this generation makes escaping from the plague of toxic productivity quite difficult. Growing up we have all heard the stories of the business person working 60+ hours a week to bring his dreams to fruition. This mentality has influenced our entire generation. Working hard should always produce tangible results, right? Well, not exactly. As someone that lives with IBD, overworking myself can have dire consequences. Stress and anxiety are common triggers for people living with IBD, so it can be exhausting to focus on extracurriculars, staying social, maintaining good grades, and overall performing “optimally” while you’re inches away from a flare up. Our culture’s ingrained toxic productivity can be seen as the genesis of this behavior. I regularly catch myself being filled with disappointment that my illness prevents me from working at the capacity that I deem as optimal. Blaming myself for the pressures that our society puts on this generation only adds fuel to the fire, but never addresses the true issue, which is our ingrained idea of hustle culture.
As young chronically ill people, we must stay aware about never pushing our boundaries and our illnesses in the name of productivity. Productivity is a wolf in sheep’s clothing; it seems innocent enough until it comes and bites us, and that bite for many of us is a flare. It is never a moral failing if you aren't able to operate at the same capacity as your pre-diagnosed self or other able bodied individuals. As chronically ill people, we have so many unique challenges that we must acknowledge and honor. Here is a metaphor that I often remind myself of:
“We are all running a race, and some people are completing laps in 7 minutes, and others are completing laps in 20 minutes. Some may have to stop to breathe, sit and take a brief rest, or even leave to grab water, but the timing doesn't matter, the effort and intention does. All effort is valid.”
In the metaphor above, the race represents toxic productivity and the one’s completing the laps in 20 minutes who have to frequently stop represents chronically ill people. Giving into the pressures of hustle culture and toxic productivity will only reinforce the cycle. So, for the college student that lives with IBD or other chronic illnesses, such as myself, who is putting excess amounts of pressure on themselves to excel in every facet of life, try to be conscious of allowing yourself the space to rest and recharge. “Rise and grind'' is hard to do when the rising part is the issue. Glamorizing and internalizing the generational curse that is hustle culture and toxic productivity can cause irreparable harm to ourselves. Remember, work does not equal self worth.
So, when you’re in bed trying to get rest and all of your responsibilities and the ghosts of toxic productivity are whispering in your ear, try your hardest to ignore those voices, turn the other direction, and get that well deserved rest.
Intestine Resection Experience in an IBD Patient
Many individuals who face inflammatory bowel disease will require surgery at some point throughout their lifetime. There are numerous reasons why an individual may need surgery such as abscesses, fistulas, scar tissue, active disease, perforations and many more ailments. Through my personal experience, I would like to share some tips to help you prepare for your experience with intestine resection surgery.
My intestine resection took place during the month of June in 2020 due to scar tissue narrowing my ileum, as well as some remaining active inflammation. During surgery, my ileum and a section of my large intestine were removed and my small intestine was then reconnected to my large intestine through a laparoscopic procedure. Enduring a surgery during the COVID-19 pandemic led me to experience a whirlwind of emotions. To begin, my original surgery date of May 2020 was postponed; however I was lucky to be able to receive it in June. During this time, hospitals in Ontario prohibited any visitors for adult patients, so unfortunately I was unable to have any visitors during my hospital stay of four days. I was so incredibly nervous to undergo a major surgery for the first time and knowing that I wouldn’t have any in-person contact with my loved ones, made the experience even more frightening. I knew that I would have to be my own advocate while in such a vulnerable position, a daunting feeling that made me quite nervous. Despite the fact I had many fears, I am happy I underwent surgery. I have recovered and continue to feel better than ever. During my hospital stay, I was taken care of by my colorectal surgeon and a wonderful team of nurses, and although I couldn’t wait to return home, I felt comfortable and secure while recovering in the hospital.
Receiving a surgery as serious as an intestine resection can seem terrifying, and trust me - I was terrified. To ease my mind and fill me with the confidence I needed to undergo this procedure, I fully immersed myself in taking great care of my physical and mental health. Physically, I made it a priority to get extra sleep, stretch often, go for walks when my body had enough energy, and made sure that I was eating nourishing foods. Mentally, I talked about my fears with my medical teams and loved ones, saw a therapist to learn coping techniques and made it a priority to journal daily. I also carefully and strategically packed a hospital bag with items that I knew would bring me comfort and make my hospital stay as easy as possible. Below are the items that I used daily during my stay.
Hospital Bag Check-List:
Night gowns or oversized T-shirts (pack comfy clothes that don’t put pressure on your abdomen)
Loose underwear
Extension cord and chargers for phone
Face wipes (it will be hard to shower!)
3-ply toilet paper (hospital 1-ply toilet paper in the WORST)
Stuffed animal to cuddle
Cozy blanket and pillow case
Easy to put on slippers (you won’t be able to bend down and they are great for walking the halls)
Perishable snacks if you require a special diet (or don’t like hospital food)
Anything else that will bring you comfort or joy
Before my surgery, I was searching everywhere online to gain insight on what my hospital experience might be like and I was unable to find many resources. I hope by sharing my personal experience in an Ontario hospital during the COVID-19 pandemic will provide comfort and ease the nerves of other IBD warriors going through a similar experience.
The Day Before Surgery:
Remember the prep before colonoscopies? She’s back! The prep instructions I received were extremely similar to colonoscopy laxative prep, along with a large dose of antibiotics. Your medical team may prescribe you something similar or different. Either way, you’ve got this!
Hospital Check-In:
After arriving at the hospital and checking in, I was brought to a change room where I was asked to change into a gown and check my suitcase. After I had changed, I was brought to a pre-operation room where the intravenous was given. My biggest piece of advice while going through all of these steps leading up to the surgery is to express how you are feeling to your nurse and medical team. I was feeling extremely uneasy and expressed these feelings to my nurse and this prompted her to request an anti-anxiety medication from the anesthesiologist that I could take prior to walking into the operating room. Once in the operating room, I received an epidural. I was personally terrified of receiving an epidural, but I experienced zero pain from the needle! After that, it was easy. I was quickly put to sleep and before I knew it the surgery was done!
After Surgery:
Upon waking up, I felt extremely tired and out of it. I continued to sleep for hours until the nurses woke me up. They encouraged me to try to stand up and use the washroom to empty my bladder. Due to the epidural and medications I received, I felt minimal pain and my legs remained numb for a few hours. Although I did not feel as if I was in pain, I could make out feelings of soreness within my abdomen. Afterwards, I was left to rest and was allowed to start drinking fluids. My medical team encouraged me to eat the next day and I brought snacks for this specific reason.
The first three days after surgery were the worst for me in terms of pain. As someone with IBD, I was accustomed to experiencing severe pain and I was able to control this pain with only Tylenol. I’ve previously been prescribed narcotics to control the pain associated with my IBD flares, so only needing Tylenol was a win in my books! My surgeon cleared me the day after surgery to begin walking the halls and moving my body. Walking was exhausting and caused me pain but it truly helped out a lot with my recovery. I was only able to stand and walk hunched over to avoid putting pressure on my abdomen which I still can’t determine whether my mind was protecting my body or if I was really unable to stand straight. This continued for about a week and each day I was able to stand up a little taller.
Returning Home:
Once I was cleared to leave the hospital, I returned to the comforts of home where I was able to have my family care for me. Stairs were unbelievably challenging and I needed support to get up and down. I was extremely exhausted for a couple weeks post-surgery and majorly prioritized rest and recovery. My biggest advice is to have a caretaker for your first few days back at home, to help you get in and out of bed, cook meals, and shower. If you are going to be alone, sleeping on the main floor and pre-making meals before surgery would be extremely beneficial to ensure you have easy access to nourishing meals.
I found it extremely difficult to get in and out of bed - I never realized just how much I use my abs! I recommend setting up a sturdy piece of furniture by your bed, such as a chair or side table, to use to lift yourself up and out of bed with. I also found that sleeping in an upright position was much more comfortable, putting less pressure on my abdomen, causing me to stack my bed with pillows.
Please remember, it can take some time for your body to adjust to the surgery and notice results. Since I had a narrow ileum that caused blockages and poor digestion, I thought I would immediately have better digestion after surgery. My digestion is a thousand times better as I write this, but it took about a month for me to truly notice any of the improvements and benefits from the surgery and continued to notice additional improvements months following. During this time of recovery, each day my body continued to become stronger and more resilient.
I hope my personal experience receiving an intestine resection will help those of you who are preparing to undergo your own intestine resection. My hope is the advice I have given you will help relieve your nerves and guide you through the process, by giving you a better idea of what to expect. As members of the IBD community, we are strong, courageous and resilient!
How My Mental Health Was Affected by IBD
Mental health has been on my mind a lot lately. From hearing it in relation to the COVID-19 pandemic, to having conversations about the need for more resources for IBD patients, to dealing with my own experiences with depression and anxiety - mental health resources are perhaps one of the most underrated and underfunded sectors of healthcare. I realize this as I’ve gotten older, immersed myself in the medical field, and as I have utilized it for my own mental health after being diagnosed with ulcerative colitis (UC) in 2016.
I bet many of you have also dealt with IBD affecting your mental health whether you realize it or not. For most of us, we were the only person we knew who had IBD at the time we were diagnosed. Some of us may not have even heard of it until we were told after our colonoscopy or endoscopy. The world around you suddenly feels a lot busier and bigger, and you feel very small and alone. Alone, wrapped up in your thoughts, your pain, your exhaustion, your fear. None of us asked for this. What did we do to deserve this?! In the days after my colonoscopy, this thought permeated my mind and I wanted to curl up in a ball and wish it all away.
But, you can’t do that when you are a busy pre-med student working full time and taking classes! We are expected to stay strong and keep up our front that says “Everything’s fine,” when, in fact, we’re not. I had great people to talk to and that would listen to me, but I still went through a mourning process. I mourned my life before when I thought I “just had a sensitive stomach.” I mourned that fact that my diet would probably change and change again and that I maybe would have to be on immunosuppressive medication. I dreaded the future conversations that would come up when someone would ask why I had to go to the bathroom so much or why I couldn’t eat or drink something. Really, everything’s fine…
But, it’s not. CHRONIC is a word that I hoped never to hear in regard to my medical history. We now have a new label that we must carry for the rest of our lives, and it’s anything but predictable. We have to explain this diagnosis so many times we feel like it might actually define us. The reality of my UC diagnosis began to truly sink in and anxiety began to seep into my daily life. My energy and concentration was poured into reading about UC, finding a better “diet”, looking for tips on how to achieve and stay in remission, and finding some kind of outlet for my anger and frustration.
Honestly, I should have given myself a little more time to process and try to seek the help of a mental health professional. Now, I think, I should’ve thought about my IBD and mental health together rather than separately. I let myself have a little time to mourn my UC diagnosis, but I thought I needed to be strong and keep my diagnosis to myself, much like others had before me. If we don’t look sick, perhaps no one will know. Even when we try our best to be strong and adapt to this normal, our mental health often still ends up suffering.
I think it would make such a positive difference in the lives of so many if we are all equipped with a medical and mental health treatment plan after being diagnosed with IBD, because the fact of the matter is that the mental health symptoms are just as debilitating as the physical symptoms of IBD, and they’re often intertwined. We need this kind of support as we manage our diagnosis - which sometimes can land us in the hospital or needing major surgery. I can’t speak to these kinds of experiences, but they can be traumatic in their own ways. How many failed medications or pain does one endure until they receive a potentially life-changing surgery? Thinking of the mental health hurdles that my co-fellows have dealt with and shared so vulnerably leaves me in awe of their strength. When they share what they have lived through, it also makes me sad that there was not adequate mental health services available to some of them when it could have offered an outlet for some of their pain.
Even now, almost 5 years out from my diagnosis, I take medication for my depression/anxiety and have re-established a relationship with a counselor that has experience in treating clients with chronic illnesses. I still go through the peaks and valleys of life and IBD, but, now, I’m better equipped to handle the lows when they hit or when a flare affects my mood and interest in doing things. I want the mental health support that has been so instrumental to some of my healing to be more accessible and affordable for those with IBD in the near future.
I hope speaking candidly about mental health and sharing some of these reflections helps you feel less alone and more validated in what you’ve been going through. The process of untangling all of these emotions is normal when grappling with a chronic illness diagnosis and what that means for you and those you love. Everyone processes major life changes and trauma differently, but don’t be afraid to ask about mental health services when you see your GI or primary care provider. Finding the right mental health support could be the treatment you never knew you needed.
Planning with Crohn's
Stay with me for this one – I promise it won’t be as boring as it sounds! If you immediately switch off when you hear the world ‘plan’, or indeed ‘regime’ or ‘strategy’, you’re not the only one! There are, however, benefits to planning when you live with a chronic condition like Crohn’s Disease – and more importantly, if your plans become routines, then they’re more likely to become second nature, and you’ll find yourself doing those tasks subconsciously. Here, I will share some of my planning tips, which you may just find helpful. It’s all about finding what works for you so that you can manage to fit in all of the things you want to do, despite your health condition(s).
Smartphone apps
There are tons of smartphone apps available to help you keep lists, plan activities and so on! I keep it fairly simple, making use of macOS/iOS Calendar, Reminders and Notes (or the same apps on other operating devices). The calendar function is ideal for noting down all of your appointments. This helps for looking to the future, but also looking back at when and where different events occurred. The reminders app is an absolute lifeline for me. I have separate folders for different activities (e.g. university, health, work, voluntary commitments and so on). I add in activities, and a date/time (or location) reminder. This definitely helps me to keep track of everything that I need to do. If I didn’t, I would definitely forget! From a health tracking perspective, this is ideal as a reminder for booking in my next vitamin B12 injection which takes place every three months, as well as for when I need to ring up my doctor to arrange routine blood tests, when I need to self-inject my treatment, and when I need to order my repeat prescription. You may think that you’ll remember everything, but when you are busy with ‘life’, on top of ‘brain fog’ which many of us can relate to, it’s easy to forget. I know I have done that in the past, particularly when it came to self-injecting my treatment. I would remember that I need it on Tuesday for example, which would be the two-week dose period. However, I would have a busy day at college, would forget when I came home, and then in bed at night, I would suddenly remember, and think ‘I’ll have it tomorrow’. But then tomorrow became the weekend, and before I knew it, it may be a whole week later and I still hadn’t given myself my injection. I knew that was no good, but I just needed to do something about it – which I did!
Finally, Notes are brilliant! Again, I have different folders for a whole variety of different items. ‘Health’ is one of those. I use notes for keeping track of how I have been feeling, as well as for noting down points to discuss with my healthcare teams. I also use notes to keep track of discussions held with healthcare professionals, either face-to-face or over the phone. It’s just another good way to have information at your fingertips to help with your care, while the discussions are still ‘fresh’ in your head.
Scheduling in rest days
We all know what it’s like to live with a condition like Crohn’s – we have so much robbed away from us. As a result, when you are feeling on the better side, you will naturally try to fit in everything that you can. I know that I have been there! Though sometimes, it really doesn’t pay off. That’s why I try to give myself time and space to just ‘do nothing’ – because I know that’s what my body needs. In pre-pandemic times, I would avoid booking in too many back-to-back travels, so that I always had some time to recover. In the current climate, I do my best to block off certain days where I’ll have meetings, keeping overs ‘free’ to do work at my own pace, and also take it easy. It’s all about being in control, as much as possible, so that you give your body (and importantly, your mind) the time and space to breathe.
Leaving the house with everything that you need
Phone. Wallet/purse. Keys. Mask! The list goes on – but it’s really important to have everything that you need to hand. As well as the usual items that most of us require these days, I also have supplies in my backpack and car for every eventuality. This includes painkilling tablets and gel, anti-spasmodic tablets to help with cramps, laxative tablets if I notice a blockage, anti-diarrhoeal tablets if the opposite happens, lactase enzyme to help me digest products containing lactose and the RADAR key to access locked accessible toilets. This list can go on and will depend on personal circumstances. I always find it best to have everything stored in one bag, so you can ‘grab and go’. It may feel excessive, but you will thank yourself later on when you’re not caught short.
Knowing your triggers and avoiding them
Although everyone is different, we all have some kind of trigger which can worsen how we feel. For me, I know that stress is a key trigger for worsening symptoms. That’s why I try to minimise stress as much as is practically possible – although that is much easier said than done! That’s why you’ll generally see me planning to do work well in advance of deadlines, for example, and seemingly ‘being on top’ of everything. In reality, it’s much harder to do, and I do find myself rushing for deadlines still – but at least I have minimised that as much as is practically possible. I am also my own worst enemy. As a perfectionist, I place huge amounts of pressure on myself to succeed and to do everything to the very best of my abilities. While it’s a good quality to have, it isn’t when it impacts on your health. So, it’s really important to be kind to yourself, and to re-evaluate your workload if you find yourself totally swamped and feeling ill. Nothing is worth more than your health.
Do you have any other planning tips which help you to live with your condition whilst getting through life? Let us know in the comments and on social media!
What to Expect When a Loved One Gets Diagnosed with IBD
Navigating an IBD diagnosis is not easy. It can be messy and emotional and very tiring. The person diagnosed with IBD will be feeling many emotions, probably all at once. But it’s not just hard on the diagnosed individual; it can be very hard on their loved ones as well. It can be difficult to figure out what to expect and what to say and how to act when you find out someone was diagnosed with Crohn’s disease or ulcerative colitis. Hopefully this article will provide some insight into what to expect when that diagnosis happens.
The first few hours and days after your loved one gets diagnosed with IBD can be very confusing. You are processing their diagnosis, while trying to be there for them as well. While everyone processes it differently, there are likely some common reactions you can expect. Here are a few things to keep in mind:
Be prepared to simply be there for them. Whether they want to talk about it or not; whether they want you to accompany them to appointments or infusions; whether they want someone to sit with them while they are sick. And even if they don’t want any of that, make sure that they just know that you will be there if/when they do. Be there for them when they are ready to talk to you. Tell them you are there if they need anything and be ready to back it up with your actions. There is nothing worse than empty words.
Be prepared for them to become experts on their own bodies. They will become very familiar with their symptoms and will likely know when something is not right. Learn to trust that. If they tell you they think something is wrong, don’t try to argue with it.
Be willing to learn with them. For me, I read up a lot on my diagnosis. I read others’ stories, I read articles, I read medical journals. And I wanted my friends and family to understand some of what I was learning. So, be willing to read the articles they send you. Educate yourself on their disease. Don’t be afraid to be educated.
Be ready for the hard days. The days when their medication isn’t working. The days when their Prednisone is making them miserable. The days when they are in the hospital. Not every day will be hard, but some will be. So be prepared when they come. Remind your loved one that it won’t last forever.
Also be ready for the good days! The days when they find out they’re in remission. The day when they try a food they haven’t been able to eat in a while and it goes well. The days when they feel like themselves. Just as the bad days come and go, the good days will come, too.
Be ready for the doctors’ appointment. Especially when your loved one is first diagnosed and they are working to get control of the disease, there will be a lot of doctors’ visits. There will be ER visits and hospital stays. There might be infusions they have to go to on a regular basis. They may or may not want you to come. Be ready to support them either way. With COVID, they may have wanted you to come and you may not be able to. If that’s the case, try to get creative with ways to make them feel like you’re there. FaceTime them, call them, text them. Do something to make them not feel so alone.
Ultimately, be ready for a journey. It isn’t always easy and there will be really hard days. But your loved one is now part of a community that is welcoming and ready to help when they want. There will be people that they can relate to and that can understand them in ways that someone without IBD can’t understand. Encourage them to reach out to people they see on social media. Encourage them to ask questions and not be afraid to speak up. The IBD community is a great one and people are always willing to help!
Navigating a loved one’s IBD diagnosis can be a daunting thing. It is a lot to process and there is a lot of unknown. But by just being supportive and being attentive to your loved one, things will probably go a lot better than you expect them to.
Judging Symptoms with Crohn’s
Sometimes, it feels like all gastro symptoms are inflammaotry bowel disease (IBD)-related… especially being symptomatic with IBD for so long. However, it’s not always case – which can cause a great of confusion, as well as making life just that bit more complicated!
As well as Crohn’s disease, I also have gastroesophageal reflux disease (GERD), irritable bowel syndrome with constipation (IBS-C), an internal rectal prolapse and lactose intolerance. I was diagnosed with Crohn’s disease in 2008, after several years of experience gastro-related symptoms. So, at that point, I assumed that everything I had experienced was the result of Crohn’s. What I failed to realise, and what wasn’t explained very well at the time, was that I also had GERD. I was suddenly prescribed all of this medication, without being properly informed of the purpose of each different medication.
Over time, and with the right treatment, I became more informed, and I was able to get my Crohn’s disease under control, to the point where I was deemed to be in clinical remission. This was concluded by considering blood tests for inflammation (CRP and ESR), colonoscopy and gastroscopy results, small bowel MRI scan results and faecal calprotectin results, each of them done at different frequencies over different periods of time. This happened gradually over a few years, and in the process, I learned more and more about my body. However, I began to struggle with more gastro-related symptoms, which I initially thought were a Crohn’s flare, but soon realised were not exactly the same as before my Crohn’s diagnosis. I felt bloated and constipated, I had abdominal pain, and I was passing mucus. It became clear that I most likely had IBS-C. The problem I found with IBS was that there was no quick and easy fix for it – not that there has been a quick and easy fix for Crohn’s disease, but at least I was able to take some treatment which helped control the inflammation. With IBS, I felt very much in the dark. Recommendations were an anti-spasmodic to relieve cramping, laxatives to ease constipation, and avoiding foods which seemed to make me ‘worse’. I watched what I ate very closely, and soon identified certain green vegetables as a trigger, as well as milk products, which I tried to reduce.
Little did I know, but the milk products weren’t just a trigger for worsening my IBS symptoms, but I was also lactose intolerant. I was diagnosed in 2015 – some seven years after my Crohn’s diagnosis. This only happened after one doctor felt there was something else going on and decided to test for lactose intolerance and Helicobacter Pylori infection – and thank goodness they did! I’ve managed to cut most forms of lactose completely out of my diet since, and when I can’t, I have found a lactase enzyme supplement I can take immediately before eating or drinking something containing lactose, to help me avoid those unpleasant symptoms.
I thought that was going to be it when it came to gastro problems. Then, something else came along! Originally blamed on my IBS-C, I noticed I was struggling more with constipation, despite eating a balanced and healthy diet, and doing everything else ‘right’. A couple of healthcare professionals didn’t really acknowledge my perspective, and just said I need to take laxatives permanently – something which I do take, but often feels like a ‘quick fix’ or ‘cover the wound with a plaster’, without understanding the underlying reason for these changes. Many blame IBD, plus IBS for constipation, without necessarily looking further. It sometimes feels as though assumptions are an easier option in the medical world, but not for those of us living with these symptoms. Moreover, I had observed changes beyond those I had learned to notice by living with IBD and IBS-C.
Cutting a very long story short, I ended up going for a proctogram which revealed I had an internal rectal prolapse – which is basically when your rectum folds in on itself. It wasn’t the most dignifying procedure – much like most gastro-linked investigations. Dignity often goes straight out of the window! However, this finding did explain the sharp shooting pains I had been having in my rectum, as well as the mucus I had been passing, the ‘fresh’ blood I had noticed, and why it sometimes felt as though there was a physical obstruction – because there was. The verdict was ‘there’s not much we can do’ – something I think we’re all too used to hearing. There are surgical options, but they come with risks and they more or less said they would not be considering that option for somebody of my age. So, I was sent away with pelvic floor exercises, and the notion that ‘I just have to live with it’ – which I do. At least I received an answer for the symptoms I had been experiencing, even if I don’t have an answer as to ‘why’ I have a rectal prolapse. My current hypothesis is that it is something to do with hypermobility, which has consistently been overlooked – but that’s a whole different story!
All of these different symptoms, and the conditions subsequently diagnosed, have taught me so much. I have learned to really listen to what my body is telling me – which is not easy but does improve with time. I’m not always right, but my judgement certainly seems to be stronger now, after all of these years with IBD, IBS-C, GERD, a prolapse and lactose intolerance. I am much better at distinguishing as to ‘what’ is causing ‘what’ – although it’s impossible to always be ‘right’! You just tune into what you are feeling, almost like detective work. You place pieces of the puzzle together to help you build the picture of what you think is happening. Your previous experiences and your observations guide you, alongside being proactive in terms of knowing clinical indicators, recognising new triggers, stressors or symptoms, and then being proactive in seeking the right input from the right healthcare professionals. It comes more naturally after years of having to take things into your own hands to get answers. For example, I now know that the abdominal pain and cramping that I frequently experience is when I am perhaps a little constipated as a result of IBS-C and my internal rectal prolapse; so I adjust certain parts of my diet and take additional laxatives when I begin to notice patterns changing, early on. Likewise, the ‘whale’ noises and ‘washing machine sensation’ immediately indicate that I’ve consumed something containing lactose without realising – like the time I ate a gorgeous cheesy pizza, and then realised I hadn’t taken my lactase enzyme… I suffered for the next few hours!
These conditions, in one sense, sensitise us to be more receptive to how our bodies work. I don’t think I would have been as knowledgeable or as ‘switched on’ as I am if I hadn’t been diagnosed with them – and I wish more people recognised this, particularly certain healthcare professionals. I often have grievances with professionals who rely solely on certain clinical indicators for disease remission. For example, those who just use CRP as an indicator as to whether you are in remission or not. This has happened to me in the past when I was evidently in the middle of an IBD flare, but at that point in time, I was not confident at self-managing my health. As it turned out, my faecal calprotectin was off the scale, and so some additional treatment helped me out immensely. What did I learn? Nobody knows my body better than myself. Healthcare professionals can help me the most when they listen to what I am saying, acknowledge my expertise, and then work with me to identify what is really happening, and then plan with me as to what to do to help manage symptoms so that I can get on with my life, and most importantly, have a good quality of life. So, when anybody questions what you are thinking or feeling, remind them of this point, and hopefully, they will change their approach so that it is supportive, rather than a hindrance.
Thoughts on IBD in the Workplace
Please provide your most recent job history. Done. Proceed to the next page. Do you have a disability that you would voluntarily like to disclose? This can include autism, blindness, cerebral palsy, missing limbs, autoimmune conditions like lupus, gastrointestinal diseases like Crohn’s disease or IBS…I blinked, and stopped. What did I just read?
In the past, I had always checked No, I don’t have a disability or history of disability. But now, as I start to look for Physician Assistant (PA) jobs, I can’t ignore the fact that I live with ulcerative colitis (UC) and flares can rear their ugly heads even when I take the best care of myself. I never had to sit and ponder this question before. Because of the way disabilities are viewed by most people, stigma swirls around it, leaving previously unaffected people like me unaware and uneducated about progress being made and the struggles still faced in the workplace. Disabilities are commonly viewed with negative connotations - several of my coworkers and other colleagues that live with chronic illness and/or disabilities have highlighted this and spoken powerfully against this negativity. Living with a disability doesn’t mean that you don’t have as much to offer. The people I’ve met through the chronic illness and disability community are some of the most resilient, creative leaders I know. We face our challenges and continue living and advocating against all that is physically or mentally against us - we have to draw incredible strength and grow up sooner and in ways that most others don’t.
However, I still struggled with multiple emotions as I sat, mulling my thoughts, stuck on this page of a job application. I have never considered myself as a person “who has a disability.” I felt guilty - would those with disabilities think that I don’t support them since I don’t want to group myself with them, giving myself another label that’s often viewed as weak? Am I misrepresenting those who do have disabilities because my UC has been so mild and I am largely functional? I felt that I don’t belong in the “disability group”, but I also can’t deny that I have a chronic illness that can be disabling in a variety of ways. I definitely consider myself lucky and blessed, but I know that my UC can change throughout my life and potentially become more difficult to control. I struggled to work through these thoughts, but then thought about how my growth this year from being more involved with advocacy has given me tools to advocate for myself and to continue learning from this community.
My options were:
Yes, I have a disability, or have a history/record of having a disability
No, I don’t have a disability, or a history/record of having a disability
I don’t wish to answer
What should I choose? It had to be either #1 or #3. I couldn’t lie - I was more afraid that it would not go over well if I did get the job and had to bring up my UC later to my employer. But then, if I marked “yes”, could that jeopardize the chances of me getting interviewed or getting a job? I’ve heard awful stories about those who hid their disability from their employer because they knew it would affect them being hired or even interviewed. Luckily, I was working with another healthcare provider who had been diagnosed with lupus over the past year and was also learning how to navigate her chronic illness in the work environment. I asked her what she thought and we ended up having a candid conversation - I realized that if marking “yes” caused me to not get an interview or a job, then that job wouldn’t have been supportive enough for me anyway. Perhaps this is my stubborn streak coming through, but I hope that working in the medical field will hopefully make potential employers more understanding. However, I know that the stigma that encircles chronic illness and disability still permeates the workplace, and this fact will stay on my mind throughout my job search.
In the end, I did mark “yes.” It is more important to me to have the chance to advocate for myself and be supported rather than hiding my diagnosis out of potential embarrassment or fear of how I would be treated because of it. Maybe this will backfire, but by being up front about my UC, I’ll feel more comfortable in my workplace. I hope that I’ll be supported enough to communicate any issues I’m having or if I do end up needing some sort of accommodation in the future. I’m very excited about applying for jobs and starting this new chapter in my life and career as a PA, but I still have much to learn about disability in the workplace. I hope by learning to navigate these waters, I can help others who may be in the same situation - questioning if they fall into the disability category or not, wondering how they should approach disclosing (or not disclosing) their condition to their employer. Since the US just hit the 30th anniversary of the Americans with Disabilities Act, I also plan to continue to educate myself and learn more about the disability community in conjunction with chronic illness. We should never have to choose between our career and our health, and I hope I can join many others who are working to make this a reality for all who are affected by chronic illness or disability.